Research carried out at the University of Zürich has revealed that the immune protein interleukin (IL)-12 does not cause the autoimmune skin condition psoriasis, but is actually protective against the condition.
“Our findings indicate that blocking IL-12 is not advisable, and such drugs should therefore no longer be used to treat psoriasis patients,” says Pascale Zwicky, PhD student at the university and first author of the study, in a press statement.
IL-12 is just one of a number of interleukin proteins that play a range of different roles in regulating the immune system and inflammation. IL-12 shares a section of sequence, subunit p40, with IL-23. The p40 subunit is linked to inflammatory diseases such as psoriasis and mice that lack it are resistant to a number of different diseases.
This led to the development of biologic drugs such as ustekinumab that could block the activity of p40 for treatment of psoriasis and other autoimmune conditions. At the time it was assumed that IL-12 was responsible for triggering the onset of psoriasis, but further information now suggests that IL-23 is the trigger and IL-12 plays a more protective role in regulating inflammation.
This is supported by the fact that newer monoclonal antibodies guselkumab and risankizumab, which more specifically block IL-23 and not IL-12, are more effective treatments for psoriasis.
“However, although the protective role of IL-12 in preclinical models of psoriasis has been established, the cellular targets and mechanisms underpinning the protective features of IL-12 remain to be determined,” write the authors in the journal Science Immunology.
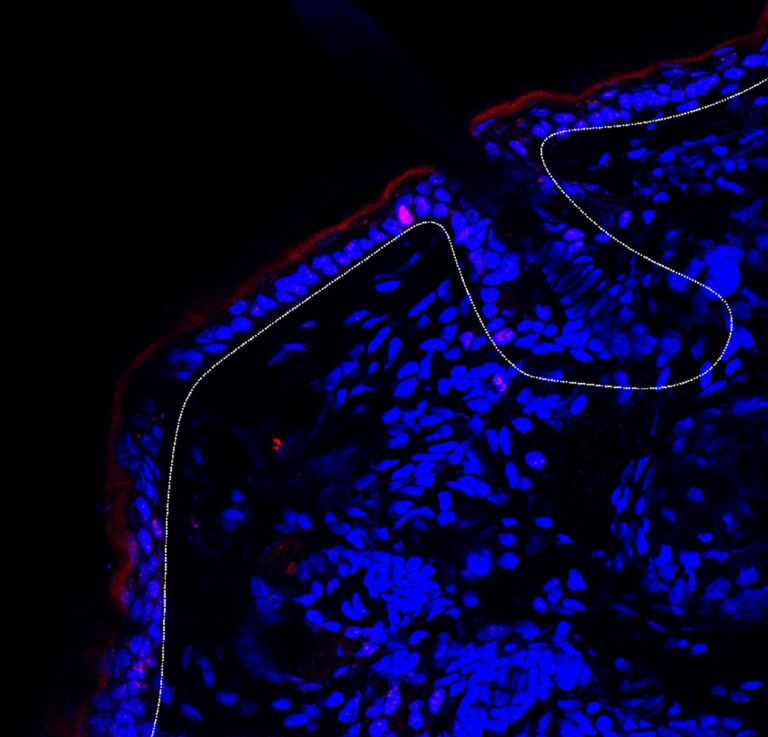
To investigate the role of IL-12 in psoriasis further, they carried out an investigation in a mouse model of the condition, as well as in human tissue samples. They found that many skin cells have IL-12 receptors and that the protein plays an important regulatory role.
“Interleukin-12 is essential for the normal, physiological function of keratinocytes. For example, it prevents the increased cell division observed in psoriasis,” explains Sarah Mundt, a group leader based at the Institute of Experimental Immunology at the University of Zürich and co-lead researcher on the study. Blocking IL-12 in keratinocytes actually increased inflammation, confirming its protective role.
“The observation that IL-12 has a profound effect on the affected tissue stroma supports the speculation that psoriasis is not primarily the result of immune dysfunction but may be a consequence of altered tissue homeostasis,” write the authors.
The researchers say that their results show that patients with psoriasis should not be prescribed monoclonal antibodies that block the activity of IL-12 as well as IL-23. Drugs that impact both proteins are still prescribed for other autoimmune conditions such as chronic inflammatory bowel diseases and psoriatic arthritis.
“In these diseases, the role of interleukin-12 has not yet been sufficiently studied. But here, too, a protective role of the messenger substance is possible,” says Burkhard Becher, a professor at the university and co-lead investigator of the study.