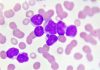
Triple-negative breast cancer (TNBC) is notoriously difficult to treat because it lacks the receptors for estrogen, progesterone, and the growth factor HER2, all three of which can be targeted with effective cancer therapies. Standard chemotherapy regimens provide limited benefit against TNBC, and patients with metastatic disease have a poor prognosis and short survival.
Now, researchers at Massachusetts General Hospital (MGH) say they have identified, for the first, time how a highly aggressive form of breast cancer can evade one of the most powerful and effective drugs used to treat it. Reporting their findings in Cancer Discovery, the team believes its work could help improve therapy and ultimately prolong survival for patients with metastatic TNBC.
But as Aditya Bardia, MD, from the Mass General Cancer Center, and colleagues previously reported, patients with metastatic TNBC treated in a large clinical trial with the compound sacituzumab govitecan (SG; tradename Trovdely) lived nearly twice as long as patients treated with chemotherapy alone.
Therapeutic is an antibody-drug conjugate
SG is an antibody-drug conjugate, consisting of the antibody hRS7 targeted to the Trop2 receptor found on the surface of most breast cancer cells, plus a cancer-killing compound known as SN-38 (topoisomerase I inhibitor), which is designed to specifically seek out breast cancer cells and deliver SN-38 as its toxic payload.
Nevertheless, some patients with metastatic TNBC either do not benefit from treatment with SG or have an initial response to treatment but then develop drug-resistant disease.
Now, Bardia, with Leif Ellisen M.D., Ph.D., director of Breast Medical Oncology at Mass General Cancer Center, and MGH colleagues, report that they have identified for the first time two separate alterations in the genome of TNBC cells that allow them to develop resistance to the antibody-drug conjugate in patients with triple-negative breast cancer.
“We sought to identify mechanisms of SG resistance through RNA and whole-exome sequencing of pre-treatment and post-progression specimens. One patient exhibiting de novo progression lacked TROP2 expression, in contrast to robust TROP2 expression and focal genomic amplification of TACSTD2/TROP2 observed in a patient with a deep, prolonged response to SG,” write the investigators.
“Analysis of acquired genomic resistance in this case revealed one phylogenetic branch harboring a canonical TOP1 E418K resistance mutation and subsequent frameshift TOP1 mutation, while a distinct branch exhibited a novel TACSTD2/TROP2 T256R missense mutation. Reconstitution experiments demonstrated that TROP2 T256R confers SG resistance via defective plasma membrane localization and reduced cell surface binding by hRS7.”
“These findings highlight parallel genomic alterations in both antibody and payload targets associated with resistance to SG.”
“In terms of de novo resistance, the data supported prior studies which suggested that the complete absence of Trop2 could be an important predictor of primary resistance,” says Ellisen. “But the really remarkable part of the study had to do with acquired resistance.”
When they studied the genomic profiles of tissues sampled both before treatment and after disease progression, they found that in multiple metastatic lesions from one woman who had an initial robust response to SG but later had disease progression and died from the disease, there were different molecular mechanisms of resistance in different metastatic lesions.
“All of the resistance mechanisms were driven by genetic changes in the metastatic tumor cells that were not present in the primary tumor. Remarkably, in one set of metastatic lesions there was a mutation in the Trop2 target of the antibody, and in another set of lesions there was actually a mutation in the target of the cytotoxic payload,” continues Ellisen.
“This is the first report describing mechanisms of acquired resistance to sacituzumab govitecan,” adds Bardia. “The findings have potential clinical significance for guiding antibody-drug conjugate sequencing for patients with breast cancer.”