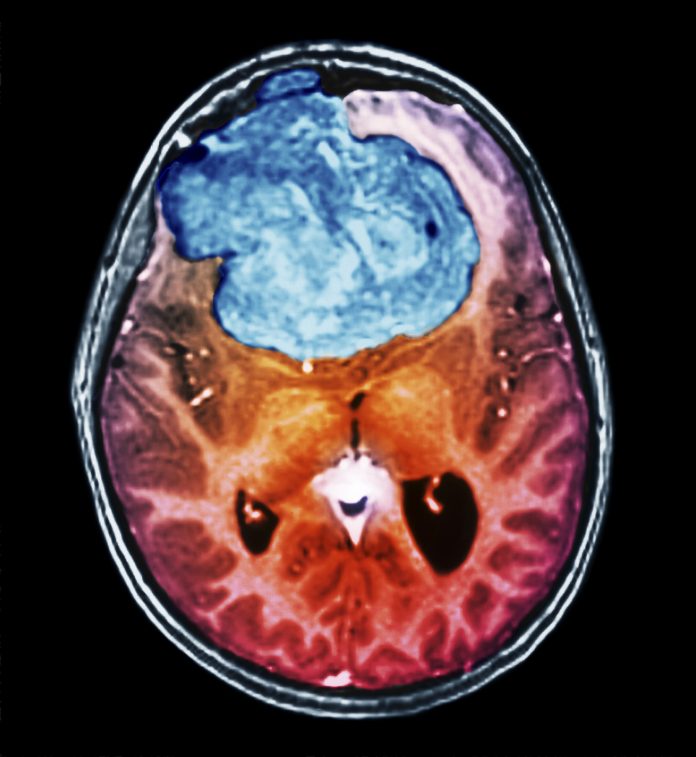
Reliably predicting whether the most common primary brain tumor, meningioma, will recur or remain benign has not been easy. Now, a team of researchers from Baylor College of Medicine and the Jan and Dan Duncan Neurological Research Institute (Duncan NRI) at Texas Children’s Hospital report that molecular analysis of 365 meningiomas has classified three different types of the disease and found one of them as most often malignant.
The current classification of these tumors from the World Health Organization divides meningiomas into three categories, grade I for a benign tumor, grade II for an atypical tumor, and grade III for a malignant tumor. According to Akash Patel, a neurosurgeon and specialist in meningioma at Baylor St. Luke’s Medical Center the WHO grading has some success for predicting tumor recurrence, but could also be improved upon.
“For instance, WHO grade II and III tumors tend to recur, but we also have seen patients with grade II meningioma whose tumors have a more benign course,” said Patel, who also is an associate professor of neurosurgery at Baylor and an investigator at the Duncan NRI. “On the other hand, a portion of grade I tumors, which are generally cured with surgery, recur despite complete resection and benign microscopic features. It seems that the way we are looking at meningioma could benefit from reevaluation, and this inspired us to continue searching for evidence supporting a better way to predict tumor behavior.”
In prior research, Patel and his colleagues examined meningioma tumors at the genetic rather than cellular level, using three profiling approaches: whole exome sequencing, RNA sequencing, and gene copy number variations. They identified three distinct groups of meningioma which the team dubbed A, B, and C as didn’t correspond with the WHO grading system. Group C tumors had a remarkably worse clinical course than group A or B tumors. Classifying the tumors using these molecular profiling techniques enabled better prediction of tumor behavior than the WHO system.
In the current study, Patel and his colleagues compared their meningioma molecular profiling approach with others that used DNA methylation to classify tumors.
“We conducted DNA methylation profiling of the tumors we had already looked at in our previous study to determine whether these different methodologies for classifying tumors were finding the same biological groups,” Patel said. “We found that, regardless of what profiling approach we used—gene expression or DNA methylation—we always found the same molecular groups.”
Continuing the study, the researchers then investigated whether DNA methylation or gene copy number variation was having the dominant effect on the gene expression profile in these groups. First author on the research, Jim Bayley, spent a year creating a mathematical model, the partial least squares regression model to find the answer.
Using this model, the researchers can say that, for a particular gene, its expression profile is highly correlated with its methylation profile, which suggests that the expression of that gene is probably regulated by methylation. For other genes, the gene’s expression profile may be regulated by copy number variation, not by methylation.
In the final part of the study, the investigators set out to understand what was driving the gene expression profile of the malignant group C tumors, the ones with the worst outcomes.
“We found that the more aggressive tumors tended to be more influenced by gene copy number losses, particularly chromosome 1p loss, which we see in the vast majority of the group C tumors,” Patel said. “The C group is marked by chromosomal instability, meaning these tumors have a higher tendency to add or lose entire chromosomes or sections of them, which affects the gene expression profile.”
The team suggests that this new classification approach will have implications for patients with meningiomas and how they are treated and also to better understand the more aggressive forms of the disease
“At the moment, the standard of care is to remove the tumor and counsel the patient. Identifying these groups provides patients with better prognostication,” Patel said. “Our study and those from other groups over the last few years have set the stage for a molecular classification of meningiomas. For other tumors, gliomas and medulloblastomas, molecular classification has replaced the traditional histopathological classification. We hope that in the next few years it will become standard to use molecular data to classify meningiomas, too.”