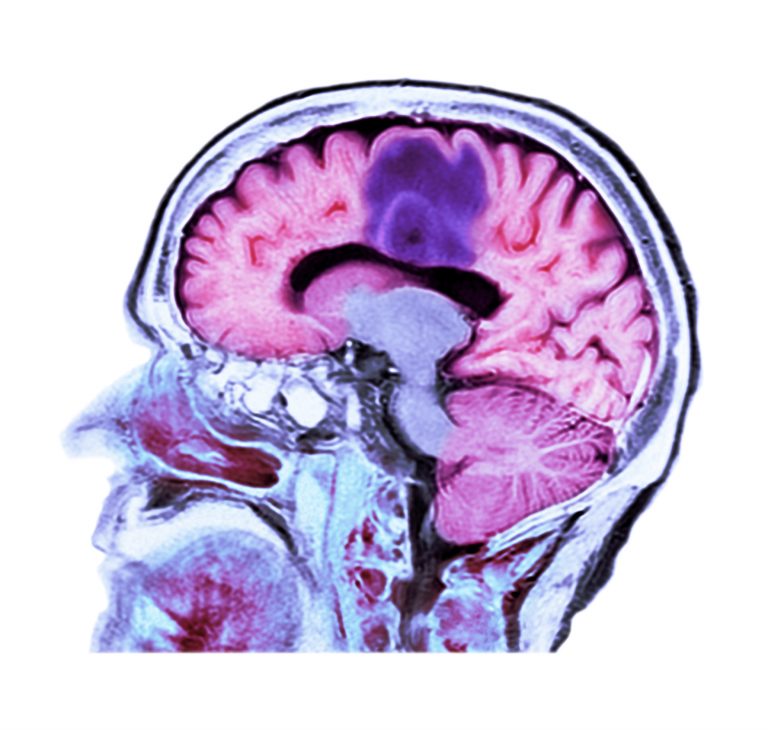
A deeper understanding of how cancer initiates, develops, and acquires resistance to treatment hinges, in part, on probing deeper into cancer stem cell biology. For glioblastoma, the most common adult primary brain cancer, this understanding is limited. Now, a study uncovers a cancer cell hierarchy that originates from a single cancer cell type, which can be targeted to slow cancer growth.
The study, which is the largest ever single-cancer cell RNA sequencing project, included 55,000 glioblastoma cells and 20,000 normal brain cells. The researchers compared the lineage hierarchy of the developing human brain to the transcriptome of cancer cells. The team found that there are five main cancer cell types within each tumor, and these cancer cell types are similar to the cell types that are in the normal human brain.
For the first time, researchers detected what they describe as a progenitor glioblastoma stem cell (GSC)—a cell type from which all other cancer cells develop. They showed a cellular hierarchical organization to the cancer which originates from progenitor GSCs.
The results are published in the paper, “Single-cell RNA-seq reveals that glioblastoma recapitulates a normal neurodevelopmental hierarchy,” in Nature Communications.
The authors wrote that they found “a conserved neural tri-lineage cancer hierarchy centered around glial progenitor-like cells.” They noted that “this progenitor population contains the majority of the cancer’s cycling cells, and, using RNA velocity, is often the originator of the other cell types.”
The team found that progenitor GSCs divided much more than the mature cancer cells and make up the vast majority of dividing cells in the tumor, despite making up a relatively small proportion of the total tumor. These rapidly dividing cells are the earliest detectable cancer cells in the hierarchy and so make a promising target for therapy.
After identifying molecular vulnerabilities in progenitor GSCs, the researchers then targeted these and found that progenitor GSC survival and proliferation decreased as a result. In preclinical disease models, this reduced tumor growth and increased survival.
“Our work has gone a long way to resolve the complexity of glioblastoma heterogeneity, and provides a new framework to reconsider the nature of glioblastoma,” said Kevin Petrecca, MD, PhD, a neurosurgeon and brain cancer researcher at The Neuro (Montreal Neurological Institute and Hospital) of McGill University.
“As part of this work, our study also shows, in contrast to decades-long dogma, that glioblastoma stem cells are the most rapidly dividing cancer cells in the tumor, and we identified new ways to target these cells. There is still much work to be done. Understanding how these cancer cells interact with the cancer microenvironment is not well understood in this disease, but this study serves as a good starting point to begin to understand how glioblastoma originates and evolves prior to treatments.”
In conclusion, the team created a hierarchal map that may be used to identify therapeutic targets specific to progenitor cancer stem cells. Their analyses, they said, “show that normal brain development reconciles glioblastoma development, suggests a possible origin for glioblastoma hierarchy, and helps to identify cancer stem cell-specific targets.”