A new study finds that chemotherapy drugs known as microtubule poisons do not work the way researchers have suspected for decades. Earlier studies showed that one microtubule drug, paclitaxel, works by interfering with mitosis to kill cancer cells though it does not stop the mitotic process entirely. This study confirms that other microtubule drugs, eribulin and vinorelbine, act in the same way. The research is published in PLOS Biology.
“Once we learned that paclitaxel is not arresting mitosis in cancer cells, we realized we needed to rethink how other microtubule poisons were acting,” explains study author Beth Weaver of the University of Wisconsin. “It turns out, they mess up mitosis just like paclitaxel.” These drugs alter mitosis—sometimes enough to cause new cancer cells to die and the disease to regress.
A class of chemotherapy drugs, microtubule-targeted agents are commonly used for cancer treatment, though as many as half of treated patients do not benefit. These findings may help explain why attempts to find new chemo drugs based solely on stopping cellular division have been so disappointing.
Researchers have long sought to develop other therapies that mimic what they believe the drugs do. “There’s still a lot of the scientific community that’s investigating mitotic arrest as a mechanism to kill tumors,” Weaver says, whose team wanted to dig deeper into the drugs’ mechanisms.
To get at that answer, the research team studied tumor samples taken from breast cancer patients who received standard anti-microtubule chemotherapy at the UW Carbone Cancer Center.
They measured how much of the drugs made it into the tumors and studied how the tumor cells responded. They found that while the cells continued to divide after being exposed to the drug, they did so abnormally. This abnormal division can lead to tumor cell death.
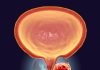
Normally, a cell’s chromosomes are duplicated before the two identical sets migrate to opposite ends of the cell mitosis in a process called chromosomal segregation. One set of chromosomes is sorted into each of two new cells.
This migration occurs because the chromosomes are attached to a cellular machine known as the mitotic spindle. Spindles are made from cellular building blocks called microtubules. Normal spindles have two ends, known as spindle poles.
Weaver and her colleagues found that paclitaxel and other microtubule poisons cause abnormalities that lead cells to form three, four or sometimes five poles during mitosis even as they continue to make just one copy of chromosomes. These poles then attract the two complete sets of chromosomes in more than two directions, scrambling the genome.
“Now that we know how they are working that puts us in a much better position to come up with a biomarker to predict which patient is going to benefit or not, potentially saving time and unnecessary side effects,” Weaver explains.
In addition, now that the drugs’ mechanism of action is better understood, Weaver believes that puts researchers in a much better position to develop additional drugs that will sensitize the resistant tumors. Her team has already made progress in that area. “Even if we have the perfect biomarker, only about half of patients are going to benefit from these drugs,” she says. “So, we need to combine these microtubule poisons with other drugs so more patients will benefit.”
The study suggests that focusing on drugs that arrest cells in mitosis is outdated thinking. ”It’s not the way forward,” Weaver adds. “We need to change our tactics that instead of trying to arrest cells in mitosis, let’s screw it up more and make it worse. That is going to kill off the tumor cells and help the patient.”
Weaver adds that researchers are now in a much better position to optimize the efficacy of chemotherapy drugs like paclitaxel and really convert them from just standard generic chemotherapy. “It’s a way to pursue personalized medicine if we can develop a biomarker of response and a way to sensitize patients to these commonly used cancer drugs.”