In a landmark moment for sickle cell disease treatment and CRISPR, two gene therapies were approved for the condition by the U.S. FDA. One of them,Vertex and CRISPR Therapeutics’ Casgevy (exagamglogene autotemcel [exa-cel]), is the first ever FDA approved CRISPR/Cas9 genome-edited cell therapy. Simultaneously, Bluebird Bio received the FDA OK for Lyfgenia, its gene therapy for sickle cell.
Bluebird said their treatment would come with a $3.1 million price tag, compared with the $2.2 million price for Casgevy. This approval also marks Bluebird’s third ex vivo gene therapy approved by the FDA for a rare genetic disease and second FDA approval for an inherited hemoglobin disorder.
Last month, the U.K. Medicines and Healthcare products Regulatory Agency (MHRA) was first to grant conditional marketing authorization for Casgevy for the treatment of sickle cell disease and transfusion-dependent beta thalassemia (TDT). The use of Casgevy for the treatment of TDT in the U.S. remains investigational.
Casgevy is a genome-edited cellular therapy consisting of autologous CD34+ hematopoietic stem cells edited by CRISPR/Cas9 technology at the erythroid-specific enhancer region of the BCL11A gene. The treatment is given by one time administration via a hematopoietic stem cell transplant procedure where the patient’s own CD34+ cells are modified to reduce BCL11A expression in erythroid lineage cells, leading to increased fetal hemoglobin production. HbF is the form of the oxygen-carrying hemoglobin that is naturally present during fetal development, which then switches to the adult form of hemoglobin after birth.
Bluebird’s Lyfgenia (lovotibeglogene autotemcel), also known as lovo-cel, is also a one-time gene therapy and custom-designed to treat the underlying cause of sickle cell disease. It works by permanently adding a functional β-globin gene to patients’ own hematopoietic (blood) stem cells (HSCs). Durable production of adult hemoglobin with anti-sickling properties (HbAT87Q) is expected following successful engraftment. HbAT87Q has a similar oxygen-binding affinity to wild-type HbA, limits sickling of red blood cells, and has the potential to reduce vaso-occlusive events (VOEs).
Both Casgevy and Lyfgenia were approved for the treatment of sickle cell disease in patients 12 years and older with recurrent vaso-occlusive crises. Approximately 16,000 patients with SCD may be eligible for such treatment.
“When our company was founded, we had a vision to translate CRISPR technology into multiple breakthrough therapies. So, this U.S. approval of the first-ever medicine using CRISPR gene editing is breathtaking, and a truly humbling moment for me personally and for the whole organization,” said Samarth Kulkarni, PhD, chairman and chief executive officer of CRISPR Therapeutics.
The administration of Casgevy requires specialized experience in stem cell transplantation; therefore, Vertex is engaging with experienced hospitals to establishing a network of independently operated, authorized treatment centers (ATCs) throughout the U.S. to offer the treatment to patients. Almost a dozen ATCs are already activated. Additional ATCs will be activated in the coming weeks and a complete list of ATCs, including updates following approval.
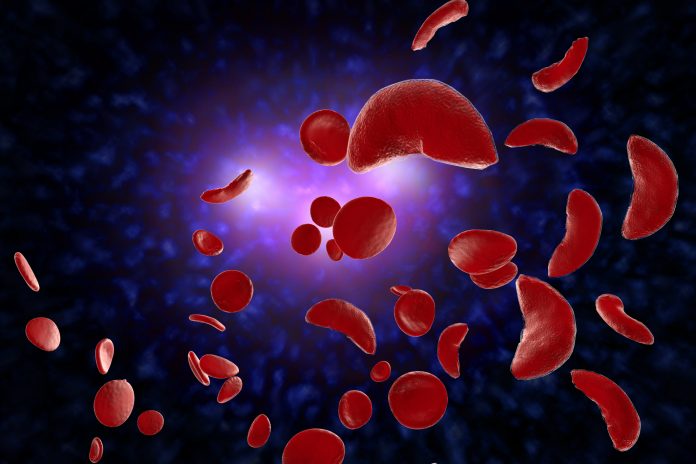
Sickle cell disease is an inherited blood disorder that affects the red blood cells. It causes severe pain, organ damage and shortened lifespan due to misshapen or “sickled” red blood cells. The clinical hallmark of SCD is VOCs, which are caused by blockages of blood vessels by sickled red blood cells and result in severe and debilitating pain that can happen anywhere in the body at any time. SCD requires a lifetime of treatment and results in a reduced life expectancy.